COVID-19 AND RHINO-ORBITAL CEREBRAL MUCORMYCOSIS
Written by Yamini Joshi
Published 27th September 2022
A paper by Dr Tarjani Dave and others from L V Prasad Eye Institute, Aditya Jyot Eye Hospital, Advanced Eye hospital and Institute, India; and Harvard Medical School, USA reviews current research on COVID-19 induced immunological alterations, hyperglycemia, and iron overload in patients, and the subsequent, explosive development of rhino-orbital cerebral mucormycosis. The authors present a survey of extant literature and discuss several parallel risk factors between the two conditions.
Rhino-orbital cerebral mucormycosis (ROCM) is a fungal infection caused by a group of opportunistic fungi called Mucorales. While Mucorales are ubiquitous, immunocompromised hosts, particularly those with uncontrolled diabetes, are at a very high risk of infection. ROCM, which is first established in the nose and sinuses, can spread rapidly to the ocular orbit and brain causing extensive damage and even death. When the infection leaves behind a characteristic eschar, a necrotic lesion around the nose and the mouth it goes by the colloquial name, ‘Black fungus.’
There is now growing evidence of COVID-19 associated Mucormycosis (CAM), where a COVID-19 infection is associated with an increased risk of secondary infection like CAM either during treatment or post-recovery. A COVID-19 infection damages the respiratory epithelium, making it easier for the Mucorales to adhere to the mucous surface. COVID-19 disrupts the body’s innate and adaptive immune systems, increases serum levels of iron in the body, and especially among those with diabetes mellitus, enhances insulin resistance and impairs immunity. All these factors are key for a fulminant mucormycosis infection too. Global research activity is now focusing on understanding the various immunopathologies that are involved in the interplay between these two conditions.
A new review in the International Journal on Orbital Disorders by Dr Tarjani Dave and other colleagues, surveys extant literature on COVID-19 Associated Mucormycosis (CAM) and summarizes the implications of CAM-induced immunopathology. The paper broadly categorizes COVID-19’s role in the establishment and progression of Mucormycosis.
The paper assembles a host of published evidence to systematically trace the path of infection within a human body and the various disruptions caused by COVID-19. It begins by noting the evidence for SARS-COV-2 induced epithelial breakdown in the respiratory lining, which leads to the adherence and subsequent invasion of fungal hyphae within the respiratory tract. Then, it presents evidence for the dysregulation of early immune responses, including that of macrophages and neutrophils. COVID-19 also leads to an increase in ferritin synthesis in the body, leading to iron overload. Excess iron impairs the adaptive immune system. All these effects are compounded in patients with hyperglycemia (either due to steroid treatment for COVID-19 or due to diabetic insulin resistance) and diabetic ketoacidosis. In fact, an environment with excess blood sugars makes more iron available to the Mucorales and aids fungal metabolism. Taken together, the paper posits, the conditions are ripe for fulminant ROCM.
‘COVID-19 precipitates a mucor infection in those who are vulnerable and have a compromised immune response,’ says Dr Tarjani Dave, lead author and consultant ophthalmologist at LVPEI. ‘In this paper, we discuss the many conducive infection pathways that are opened up for mucormycosis, after a COVID-19 infection. The many correlations and associations between the two conditions open up several new ways of understanding the aetiology and therefore the preventive strategies and possible treatment options of both conditions.’
Citation
Dave TV, Nair AG, Joseph J, Freitag SK. Immunopathology of COVID-19 and its implications in the development of rhino-orbital-cerebral mucormycosis: a major review. Orbit. 2022 Jul 20:1-10. doi: 10.1080/01676830.2022.2099428. Epub ahead of print. PMID: 35856238.
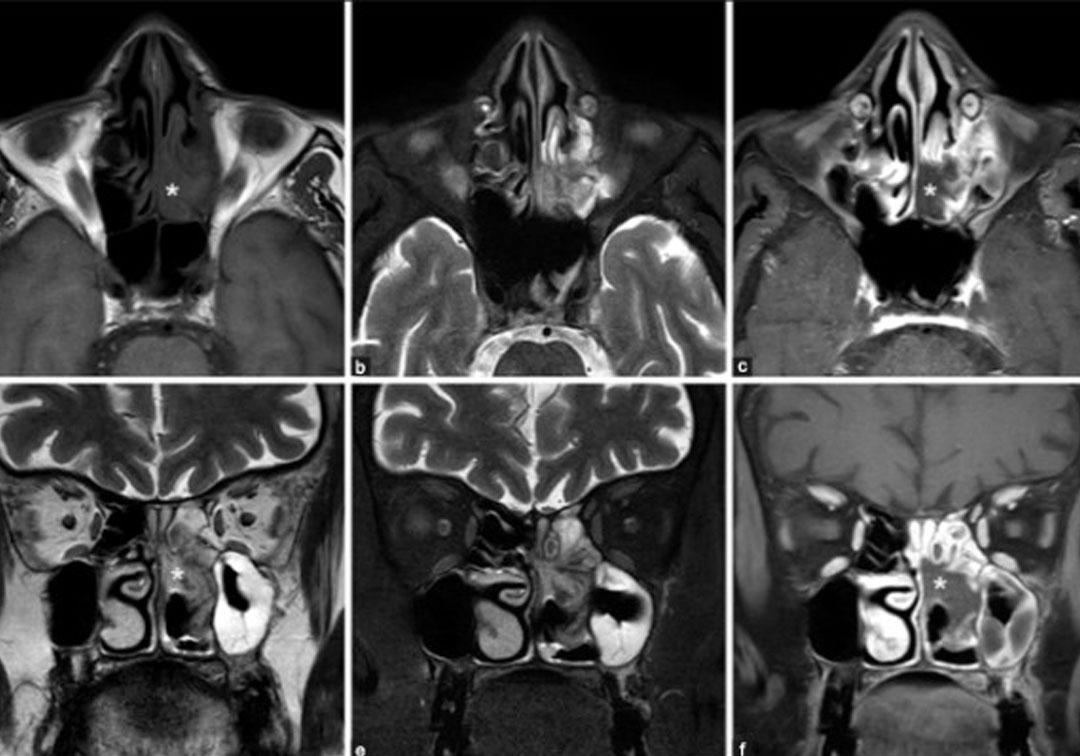
Photo credits: Sinonasal disease in ROCM; Image from the paper, ‘MRI imaging in ROCM’ by Dave et al.