Contact Lenses & Visual Outcomes after SLET
Written by Yamini Joshi
Published 25th April 2023
A paper by Drs Simmy Chaudhary, Swapna Shanbhag and others from L. V. Prasad Eye Institute evaluates the safety and efficacy of contact lenses to improve visual outcomes of patients after a simple limbal epithelial transplant (SLET) surgery. The paper looks at two types of contact lenses: rigid gas permeable (RGP) and scleral contact lenses.
The clear, outer layer of the cornea, its epithelium, is a barrier that needs regular replenishment of cells from the limbus on its border. The limbal epithelial stem cells are multipotent stem cells that ensure this supply, and act as a barrier preventing conjunctival cells from migrating onto the cornea. Damage to the limbus, mostly due to ocular burns or chemical injuries, causes a limbal stem cell deficiency (LSCD). No fresh cells are formed, and the adjoining conjunctiva spreads into the cornea leading to vision loss. When there is such an extensive loss of stem cells, a stem cell transplant may be required to restore them.
The preferred transplant technique in such circumstances, especially in developing countries, is the simple limbal epithelium transplant (SLET). SLET was developed at LVPEI. A previous study by Basu et al showed that 75.2% eyes had an increase in visual acuity at 1.5 years after autologous SLET surgery. However, the corneal stroma, its thick middle layer, may have scars after SLET impeding visual acuity. It is likely that contact lens, especially rigid gas-permeable (RGP) and scleral lens, can help improve visual acuity in such scarred eyes. But how safe are they in these circumstances? And how much improvement in visual acuity can one expect?
A new study in the Cornea journal by Dr Simmy Chaudhary, Dr Swapna Shanbhag, and others evaluates the safety, efficacy, and visual outcomes of RGP and scleral contact lens in eyes with corneal scarring after SLET. This was a retrospective, interventional study of 61 adults (median age: 22) and pediatric eyes of patients, with a majority (77%) needing SLET after chemical injury. 72% of the patients were men. All patients were fitted with RGP lens as the first option, and those with a poor RGP fit were offered scleral contact lens (56%). 29.5% of these patients did not opt for contact lens after the fitting and the median duration after the prescription was 18 months.
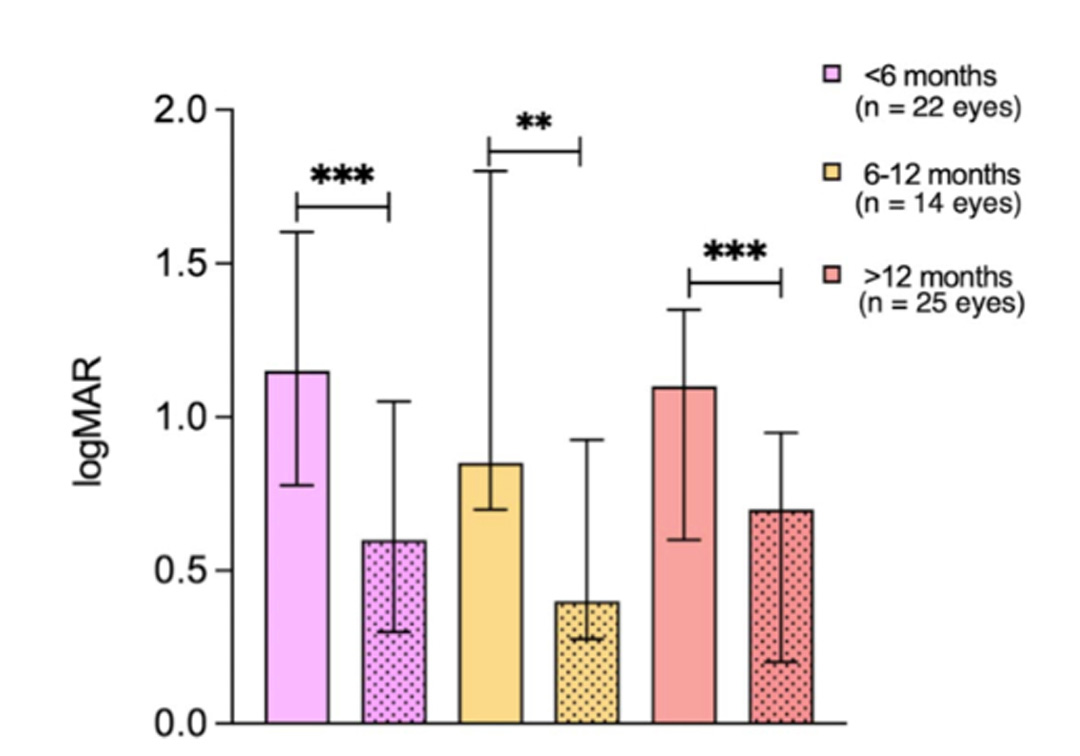
The WHO (World Health Organization) defines blindness on a logMAR scale of 1.30 to 1.80. The median best corrected visual acuity (BCVA) before SLET was 1.80 for all the patients—all were clinically blind. Post-SLET, the median BCVA improved to logMAR 1. After wearing contact lens, the median logMAR further improved to 0.6 (moderate vision impairment, per WHO). Many patients with sub-optimal BCVA after SLET may undergo penetrating keratoplasty—but at a high risk of failure. In this study, all patients saw good visual recovery with contact lens use alone. In fact, a third of the participants saw a 6-line improvement with contact lens use.
‘After SLET, although vision improves drastically in a significant subset of patients, residual corneal stromal scarring may persist, translating into reduced visual acuity. A corneal transplantation is not the best option in such cases due to an increased risk of failure. We show that contact lenses provide a safe alternative to improve visual acuity. They can be offered even three-four months after SLET,’ says Dr Swapna Shanbhag, the corresponding author for this paper and Consultant Ophthalmologist at LVPEI.
Citation
Chaudhary S, Kate A, Chappidi K, Basu S, Shanbhag SS. Safety and Efficacy of Contact Lenses in Eyes After Simple Limbal Epithelial Transplantation. Cornea. 2023 Jan 11. doi: 10.1097/ICO.0000000000003228. Epub ahead of print. PMID: 36728263.
Photo credit: Fig 3, plots depicting median BCVA after SLET (plain) and CLs (dotted) at different time points after SLET; Chaudhary et al.