Dry Eye Disease
Last updated: 5th May 2026Overview
A thin tear film nourishes, protects, and lubricates the surface the eye. It also helps in directing the light into the eye. When this tear film is disrupted, it can lead to irritation and a stinging sensation in the eye. Over time, dry eye disease (DED) can damage the cornea and impair vision. It is also important to remember that not all feeling of dryness may be DED.
Dry Eye Disease is projected to affect close to 40% of the Indian population by 2030. It is linked to screen use, medication, allergies, and pollution.
What is Dry Eye Disease?
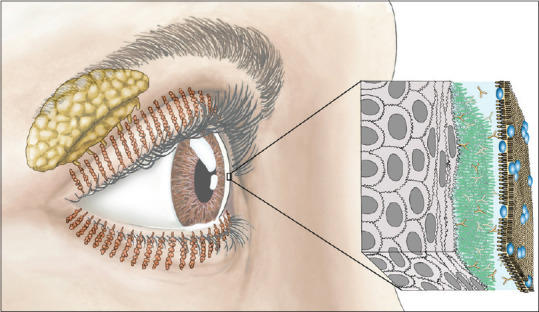
Dry Eye Disease is when the tear film that protects the eye is disrupted, leading to dry spots on the sensitive corneal layer, which is the outer layer of our eye.
The graphic above shows the location of lacrimal (Yellow, near the temple) and meibomian glands (the tunnels on the eyelids) in the eye. Also, the three components of the tear film: the lipid (brown), middle aqueous (blue), and mucin layer (green) can be seen. [1]
Human tears have 3 parts:
- an inner layer of mucous (produced by goblet cells in the conjunctiva),
- an aqueous (watery) middle layer (produced by the lacrimal glands)
- an outer lipid layer called meibum (produced by the meibomian glands)
The conjunctiva is the mucous membrane that line the eyelids and eye surface. The lacrimal glands are above our temples. Our eyelids secrete meibum through oil-secreting tunnels called meibomian glands. Meibum prevents tears from evaporating quickly and maintains the structural integrity of the tear film across the eye.
Types of dry eye
Dry eyes can be caused by excess tear evaporation or a drop in tear production. Based on that, there are two types of Dry Eye Disease:
- Evaporative dry eye
This is the most common type of dry eye disease and is increasingly found in people with prolonged digital screen use. There is a strong association between digital screen use and reduced blink rate, which could result in dry patches on the eye.
Meibomian gland dysfunction (MGD) is a leading cause of evaporative dry eye (EDE) disease. meibomian glands are blocked or damaged, the lipid layer thins down.
Cases of EDE are expected to rise with climate change and digital screen-use, but many risk factors are unknown. - Aqueous-deficient dry eye
ADDE is a set of conditions that are triggered when the lacrimal glands do not produce enough tears. About a third of all patients with Dry eyes have ADDE. Sometimes, it can just be a product of ageing. People who take antihistamines or decongestants, or other medicine that could trigger reduced tear production.
Many autoimmune conditions can also trigger ADDE, including Sjögren’s syndrome, Stevens-Johnson syndrome, rheumatoid arthritis, systemic lupus, and mucous membrane pemphigoid. [2]
What are the symptoms?
People with dry eye diseases have a range of symptoms:
- A stinging, burning sensation in the eyes
- A gritty sensation in the eyes
- A red eye with blurry vision
- A dry mouth or joint pains
- Eyes that water excessively
- Discomfort with contact lens use
- Discomfort with prolonged screen time
Prevention
- Avoid sitting directly under an air conditioner
- Keep hair dryers pointed away from your eyes
- Take eye breaks and pay attention to how you blink—a full blink matters.
- Be aware of the weather. If it is dry, take precautions
- Stop smoking
How is Dry Eye diagnosed?
At LVPEI, all patients receive a comprehensive eye exam. In addition, details of medication, systemic issues, and occupation are also taken.
- Schirmer’s eye test: This test measures tear production. Special blotting paper strips are placed in the eyes, and the wet region is measured to gauge tear volume.
- Non-invasive tear break-up time: NITBUT measures the stability of the eye’s tear film on the ocular surface. A shorter time to break the film up indicates dry eyes. It is performed using a keratography (a non-invasive tool).
- Diagnostic/Direct Assessment of Tear Secretion: DATS measures the tear volume using a fluorescein strip.
In addition, minute scars (cicatrization) on the ocular surface and other such forms of damage are noted to understand the progression of this condition.
Treatment options
Most people with dry eyes can benefit from consistent blinking, warm compress, and preventive measures including adequate rest. In addition:
- Artificial tears may be suggested to help reduce symptoms.
- Eyelid massage using special equipment can help some patients with meibomian gland dysfunction.
- Immune suppressors or modulators are offered as eye drops to reduce the impact of auto immune conditions.
- Punctal plugs are offered to preserve the tear film and not let it leak away into the nose, for those who may benefit from them.
- Scleral contact lenses are large diameter contact lens that sit on the whites of the eye and bathe the cornea in a solution that offers relief from the dryness.
- Lifestyle Adjustments: Protecting eyes, reviewing medications with your doctor, managing chronic conditions.
There are many more options and therapies that clinicians at LVPEI are exploring to help patients with the different forms of dry eye disease.
Frequently Asked Questions
Only in its very rare and severe forms. DED may impair vision and also cause impaired quality of life. Early diagnosis and treatment can help address these issues.
Excessive tears may be the body’s response to DED. A comprehensive eye exam alone can diagnose the cause and type of this condition.
This is a question for your eye doctor to answer after they thoroughly examine your eye. Different people respond differently to the many triggers that lead to DED. It is best to find out what suits you best from a professional.
Some palliative steps are available (see above). Maintaining overall health including not smoking, regulated blood sugars, and a healthy weight can be beneficial.
Systemic medication including antihistamines may trigger symptoms of DED. Please speak to an eye care professional about your symptoms, and disclose all the medication you are taking. It will help them narrow down on the triggers for DED.
